Reducing Administrative Costs Within US Healthcare: A Summary
Published in the March of 2020, the policy proposal “Reducing Administrative Costs in U.S. Health Care” by David Cutler for the Hamilton Project at Brookings outlines a detailed perspective on how to understand and alleviate the weight of unnecessary healthcare spending. He begins with a jarring statistic: the administrative costs of healthcare are twice as great as what we spend on caring for cardiovascular disease and three times as great as what we spend on caring for cancer. There must be a way to lower these costs.
The definition provided for administrative cost within the proposal is the “nonclinical costs of running a medical system,” the greatest of which fall under billing and insurance costs (BIR). BIR can include the costs of a provider verifying that a patient is eligible for services, prior authorization procedures on both provider and payer side, submitting bills and appropriate documentation, addressing denied claims, and remitting payment. While it cannot be denied that some BIR cost is necessary and unavoidable, the proposal estimates that about ½ to ⅔ of BIR is unnecessary.
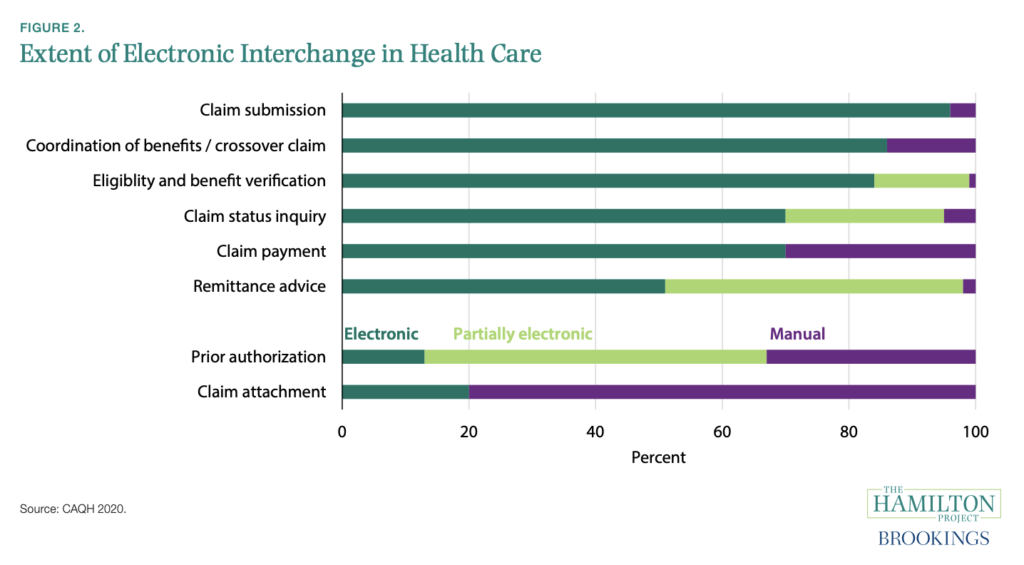
Cutler also makes an important point on the effect that increased administration can have for health care providers: “In addition to its burden on individuals, administrative costs affect the medical system in other ways. Providers dislike spending time on administrative tasks relative to time caring for patients. Provider frustration thus grows with administrative hassles. At a time when the United States needs more health-care providers, reducing administrative burden is one way to free up time for providing care (and possibly delay retirements).” Healthcare administration increases the burden on the economy of healthcare and the providers of healthcare. (You can read more on the effect of administrative burden on physician burnout here in an article by ACEA).
After defining the challenges that arise when trying to reduce healthcare administration costs, Cutler lays out a four-part proposal in combating them. These parts are 1) establishing a clearinghouse for bill submission, 2) simplifying prior authorizations, 3) harmonizing quality reporting, and 4) enhancing data interoperability in the health-care system. We will go through them in detail below.
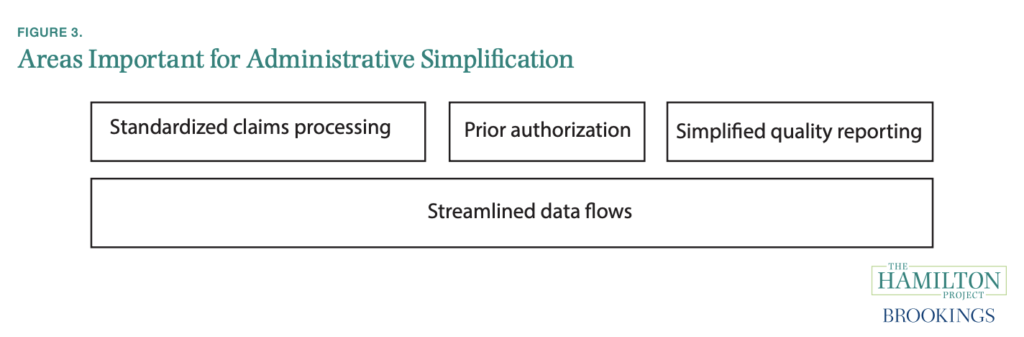
The healthcare automated clearinghouse (ACH) – or standardizing the electronic transmission of billing and claims submissions – for bill submission would be modeled after the clearinghouse used in banking. This would simplify and standardize the process of claims. Cutler defines the biggest challenge here as the necessity of near-universal participation in the ACH for it to be effective, and he follows up with the proposal to follow the Federal Reserve to require the use of those standards by any payer or provider participating in public programs. These public programs include Medicare, the ACA, federal employee insurance, VA insurance, and more. With the majority of payers in the U.S. participating in government programs, this requirement would cover them.
Prior authorization is the process of approving medical services based on clinical or economic criteria. Simplifying prior authorizations would make health care services more efficient and lower the administrative burden on physicians. Cutler proposes three steps to the simplification of prior authorization: apply rules selectively, attach a price, and automate. For example, chronic conditions would only need to be authorized every year instead of every month, lowering the administrative cost. Using a patient’s history with AI could also serve a role in when a procedure or diagnostic is appropriate or not.
The purpose of harmonizing quality reporting is to ensure that quality metrics are useful to both the patient and the provider. Cutler cites Minnesota, a state that has publicly defined quality metrics, as a good example of quality harmonization. He also proposes that quality metrics should be based on electronic medical records (EMRs), not separate records that come from clinical staff. This would contribute to the harmony of reporting metrics nationwide. He estimates that having standardized quality metrics could save around $7 billion annually.
Data interoperability, the ability to make health information flow seamlessly among providers, is the final part of Cutler’s proposal. He lists two ways to contribute to data interoperability – patients being able to directly access their medical records and having payers consolidate health information. If payers do consolidate, it would also contribute to less prior authorization as well since they will have the health information of the patients.
Cutler’s proposal is thorough and necessitates changes to a system that is deemed inefficient. With administrative spending taking up ⅓-¼ of the cost of total healthcare spending in the U.S., ways to streamline and lower costs are sorely needed. The policy proposal put forth asks for technical, political, and economic changes. By lowering the cost of administration, physicians could spend more time with patients, healthcare costs could be reduced, and patients would be more likely to access health care. These reforms, if put into place, could save the U.S. an estimated $50 billion per year.
Source: Cutler, David M. “Reducing Administrative Costs in U.S. Health Care.” The Hamilton Project, Brookings Institute, Mar. 2020, https://www.hamiltonproject.org/assets/files/Cutler_PP_LO.pdf.